The thyroid specialists at Children's Healthcare of Atlanta have advanced training in diagnosing and treating a variety of thyroid conditions in kids and teens.
Common thyroid conditions
Thyroid nodules are lumps or growths of tissue within the thyroid gland. They may be identified by a child or family member who notices a lump, found by a physician performing a physical exam, or seen incidentally when a child has an imaging test for another problem.
Most thyroid nodules are not cancer, and most thyroid nodules do not cause symptoms other than the lump in the thyroid. Most children with thyroid nodules, but not all, will have normal thyroid bloodwork. A child with a thyroid nodule should be evaluated by a thyroid specialist even if the blood tests are normal.
What causes thyroid nodules?Thyroid nodules have many causes. Family history of thyroid disease or personal history of thyroid disease, especially autoimmune thyroiditis/Hashimoto’s disease, can increase the chance of having thyroid nodules. Colloid nodules are caused by accumulation of colloid, a substance made during the production of thyroid hormone by the thyroid gland. Radiation exposure, either as part of medical care or accidental exposure due to nuclear disasters, may cause thyroid nodules. Some genetic conditions increase the chance of developing thyroid nodules. Iodine deficiency can also cause thyroid nodules, but it is not common in children who have lived most of their lives in the U.S.
What causes hyperthyroidism?
Hyperthyroidism is caused by Graves’ disease, thyroiditis, hyperfunctioning nodules or excess intake of thyroid hormone replacement. Usually, the release of thyroid hormone is controlled by the pituitary gland in the brain, but in these conditions, too much thyroid hormone is released.
Hypothyroidism is when the thyroid is not producing enough thyroid hormone. It may be due to problems with the thyroid itself or problems with the pituitary gland. Hypothyroidism may be present from birth or start later in childhood or adulthood. There are many possible causes of hypothyroidism. An endocrinologist can assist with diagnosing hypothyroidism and determining the cause.
Graves’ disease is the most common cause of overactive thyroid, also called hyperthyroidism. In this condition, the thyroid gland releases too much thyroid hormone into the blood, causing increased heart rate, increased blood pressure, increased appetite, weight loss, tremors, problems with sleep and concentration, and other symptoms. Some children will have an enlarged thyroid gland or eye problems. Most children with Graves’ disease can be treated with medication, but some will be referred for radioactive iodine therapy or thyroid surgery.
What causes Graves’ disease?
Graves’ disease occurs when the immune system causes the thyroid to become overactive. An abnormal antibody is produced by the immune system, which tells the thyroid gland to increase production of thyroid hormone. The extra hormone produced is stored in the gland, and too much hormone is released into the blood.
Thyroiditis in children usually causes hypothyroidism (low thyroid function). Most often, it is caused by an autoimmune condition. Sometimes, thyroiditis causes hyperthyroidism by damaging the thyroid tissue, allowing stored thyroid hormone to leak out into the blood. This hyperthyroidism may not be permanent and can change to hypothyroidism (low thyroid hormone levels) over time.
Both young children and adolescents can be affected by thyroid cancer, though it is more common in teens. Our team has expertise in the diagnosis and management of all types of thyroid cancer, and can guide you and your child through the treatment process every step of the way. Most pediatric thyroid cancer happens sporadically, or “out of the blue,” but we do have special follow-up for patients who might be at higher risk for developing thyroid cancer due to their other medical conditions or specific genetic syndromes. When you choose Children’s, you can expect coordinated, multispecialty evaluation and a personalized treatment plan for your child.
There is a wide range of symptoms that may occur with thyroid disease. It may present with no symptoms, or a child or teen could have symptoms of hypothyroidism or hyperthyroidism.
- Signs of hyperthyroidism include increased appetite, weight loss, tremors, problems with sleep and concentration, and other symptoms. Some children will have an enlarged thyroid gland or eye problems.
- Signs of hypothyroidism include fatigue (excessive sleepiness), sensitivity to cold, dry skin, weight gain, muscle weakness, thinning hair, depression, and excessive sleepiness.
In addition, there may be a new lump or enlargement in the thyroid gland. A mass in the thyroid may also be noticed on radiographic studies.
If your child is experiencing symptoms of hypothyroidism or hyperthyroidism, it is important to seek medical care. A child with a thyroid nodule or enlargement of the thyroid needs to be evaluated by a thyroid expert even if the blood tests are normal.
Learn more about Endocrinology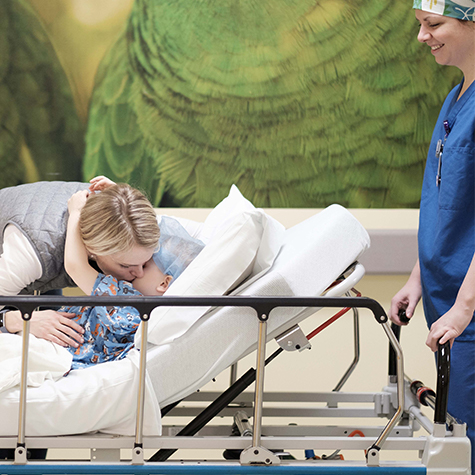
We are trained to care for your child
When you walk through our doors, you can take comfort knowing our entire staff, from pre-surgery nurses and technicians to pediatric anesthesiologists and surgeons, has been specially trained to care for your child.
The diagnosis of thyroid disease starts with an evaluation by a medical professional that includes a complete history and physical exam. Lab tests will confirm a diagnosis of hypothyroidism or hyperthyroidism. Thyroid function tests will be ordered to assess the function of the thyroid.
If there is a mass of the thyroid, your child will have an ultrasound of the thyroid and neck. The ultrasound has no radiation and is usually well tolerated by kids and teens of any age. In special cases, a CT scan or MRI may be needed.
Depending on the radiological studies, a biopsy of the mass may be needed. The biopsy, called a fine needle aspiration (FNA), in most cases will lead to a diagnosis and guide treatment. The FNA involves taking a small sample of the mass with a tiny needle. Depending on the age of the patient and other factors, your child may receive sedation for this procedure. In certain cases, genetic testing may be done on the sample. Once all the diagnostic test results are received, our specialized thyroid team will develop a plan of care.
There are several ways that our team treats thyroid disease in kids and teens.
Medication
Many times, medication can be used to help treat thyroid problems. There are medications to replace low levels of thyroid hormone, as well as medications to lower excessively high thyroid levels. Other medications may be needed to help manage symptoms in some children. However, every child is different and needs a treatment plan specific to him or her. If medication does not help, our team specializes in surgical options.
Surgery
If your child needs surgery, you will probably need to stay overnight at the hospital. Typically, this stay lasts only one night. We will help coordinate your care both in the hospital and during your outpatient follow-up visit.
Our physicians are leaders in research efforts to improve outcomes and help kids recover better after surgery. We work with specialists from many different areas to create guidelines for kids and teens who require surgery. These enhanced recovery after surgery (ERAS) guidelines have helped us reduce complications, manage post-surgery pain better and get kids home sooner.
Thyroid surgery
Some thyroid nodules may be observed over time with repeated ultrasounds and detailed physical examinations. If a nodule develops concerning features or becomes very large, or if a biopsy shows the nodule is suspicious for thyroid cancer, surgery to remove part or all of the thyroid gland may be recommended. Most pediatric thyroid cancers are treated with full removal of the thyroid gland (total thyroidectomy). Some patients may only need half of the thyroid gland removed, which is a procedure called a hemithyroidectomy. Because it is common in children for thyroid cancer to spread to nearby lymph nodes in the neck, removal of potentially involved lymph nodes is often completed at the same time.
At Children’s, thyroid surgery is performed by a small group of experts who care for a high volume of pediatric patients every year. We work hard to ensure each patient has a comprehensive, personalized surgical plan based on the best available information.
After surgery, our endocrinology team helps coordinate hormone replacement therapy and any necessary additional treatment. For patients whose thyroid cancer has spread beyond the thyroid gland, radioactive iodine therapy may be recommended to target any remaining microscopic tumor cells.
Radioactive iodine therapy
Iodine is an important ingredient in a healthy diet that your thyroid gland uses to make thyroid hormone. Because it is used only in thyroid cells, radioactive iodine (RAI) treatment may be recommended after surgery for patients whose thyroid cancer has spread beyond the thyroid gland, for patients whose cancer returns after treatment (called recurrence) or in specific cases of Graves’ disease.
RAI treatment is given by mouth and has very few side effects. Most pediatric patients stay overnight in the hospital for monitoring after the dose is given. If your child needs RAI, we will discuss the short- and long-term side effects with you before treatment. Making these decisions in advance can help reduce complications and minimize side effects for your child.
Prior to any treatment, the plan will be discussed with your child and the family. Your doctor will explain what to expect before, during and after surgery. Instructions might include how to begin a low-iodine diet, when to stop thyroid hormone therapy, and when to expect radioactive iodine whole-body scans or treatment.
Parathyroid surgery
Parathyroid glands can become overactive for a variety of reasons, leading to blood calcium levels that are too high. Many causes for abnormal parathyroid hormone levels can be treated with medications, but in some cases, medications do not help, and surgery is recommended. If this is the case, specialized imaging studies can help determine if several glands are overactive or if a single gland is responsible for the problem. Surgery is then tailored to each patient’s individual concern. Children whose blood tests show an abnormal level of parathyroid hormone should be evaluated by an endocrinologist before considering surgical treatment.
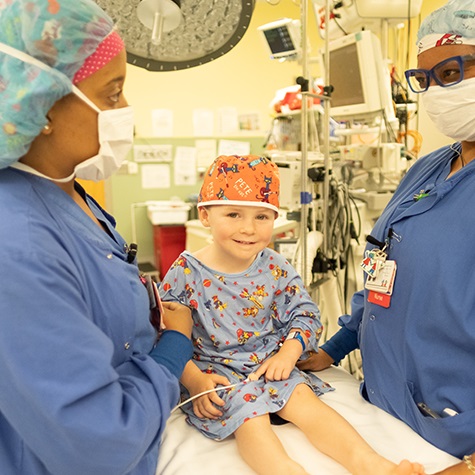
We are the first facility in Georgia with a Level 1 Children’s Surgery Verification.
We have earned Level 1 status from the American College of Surgeons for Children’s Surgery Verification—its highest designation. No other hospitals in Georgia have achieved this level. So when your child needs surgery, you can take comfort in knowing he is in a facility that meets the highest distinction.
Learn moreThe Children’s thyroid team is made up of providers with expertise across multiple specialties. Our doctors are recognized throughout the Southeast and the country, regularly contributing to academic conferences and medical education meetings related to the care of pediatric thyroid disease. Your child will have a comprehensive, multispecialty evaluation prior to any intervention to help ensure he receives the right care the first time, every time.
We also understand that care includes more than just diagnosing and treating medical conditions. Our nurses, social workers, child life specialists, therapists and volunteers understand the concerns that can arise when growing kids need to take time away from school, friends and family life to attend to medical issues. We’re here to help you navigate these concerns and get your child back to activities.
Our Thyroid Program includes physicians across numerous specialties:
Cancer
Endocrinology
General surgery
Interventional radiology
Otolaryngology
Pathology
Radiology
Contact Us 404-785-KIDS (5437)
